The Crossing Pathways Project
The Crossing Pathways Project was a Home Office funded initiative that built on Standing Together’s ‘Whole Health’ approach, as seen through the Pathfinder Project. This three-year project aimed to improve domestic abuse interventions and responses in healthcare settings to support a diverse patient population, in particular vulnerable groups who face the most barriers in disclosing? abuse or accessing services.
The purpose of the Crossing Pathways Project was to better understand the gaps in provision and barriers in healthcare settings to a coordinated response to domestic abuse disclosures, to increase the awareness and competence of healthcare professionals in responding to disclosures of domestic abuse and improve referral pathways for victim-survivors to support services.
This was achieved by working innovatively in partnership across the health and domestic abuse sectors to create sustainable change through a consistent, coordinated whole-system approach. This included developing national communities of strategy and practice to share learning and drive system-wide improvement.
The funding for this project enabled Standing Together to:
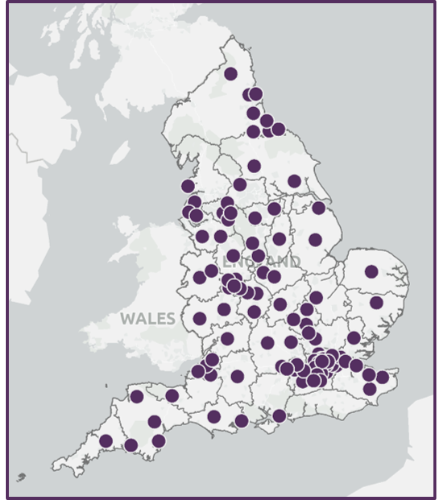
- Map the provision of health and domestic abuse services and processes throughout England and identify gaps within this provision
- Implement regional and national networks for health and domestic abuse specialists to support best practice, improve knowledge, pathways and responses for victims/survivors within healthcare settings.
- Commission 30 pilot initiatives across England through a grant funded approach.
- Develop an active survivor led approach, through the Survivor Voice Network to ensure that survivor voices were heard and held within the core of the project.
As part of this project, Standing Together commissioned 30 grant-funded services across England including Domestic Abuse Coordinators, Health IDVAs, Specialist Roles, IRISi, a Perpetrator Health Worker, an Older Persons Rural Domestic Abuse Practitioner, a Harmful Practices Trainer and a Specialist Mental Health IDVA.
Analysis conducted as part of the project evaluation indicates the average intervention cost £656 per case over an average of six months prevented high-cost critical incidents, such as domestic homicides and prolonged foster care. Early intervention saved the public sector costs exceeding £2.6 million per survivor.